Month: June 2017
Dr. P.K. Shah Featured on Life & Times of Leading Cardiologists
World-renowned cardiologist Dr. P.K. Shah arrived in the US with $8, a suitcase, and a medical degree that cost about $70. Click on the image below to learn how he … Read more
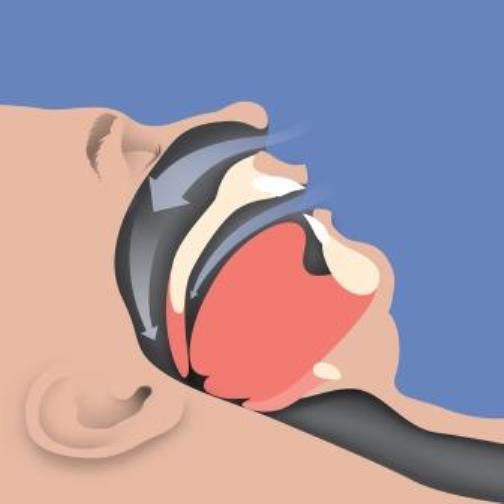
Sleep Apnea and the Heart
Sleep apnea is a serious sleep disorder that occurs when a person’s breathing is interrupted during sleep. In sleep apnea your breathing passages becomes blocked, or the muscles that control your breathing … Read more